Cracking the blood-brain barrier with magnetic nanoparticles
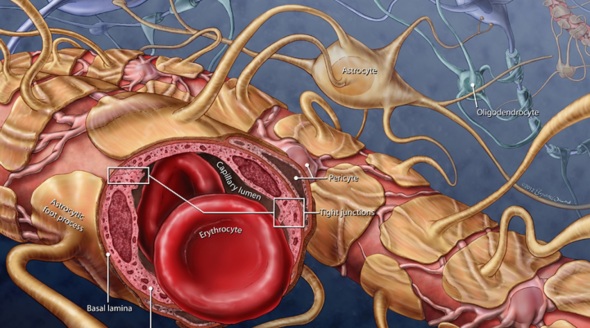
The blood-brain barrier, the thorn in the side of medicine. It makes using drugs directed for the brain ineffective at best and unusable at worst. This barrier runs inside almost all vessels in the brain and protects it from elements circulating in the blood that may be toxic to the brain. This barrier means that currently 98% of therapeutic molecules are also unable to cross to the brain. However, researchers now say magnetic nanoparticles can open the blood-brain barrier and deliver molecules directly to the brain.
“The barrier is temporary opened at a desired location for approximately 2 hours by a small elevation of the temperature generated by the nanoparticles when exposed to a radio-frequency field,” explained first author and co-inventor Seyed Nasrollah Tabatabaei.
“Our tests revealed that this technique is not associated with any inflammation of the brain. This new result could lead to a breakthrough in the way nanoparticles are used in the treatment and diagnosis of brain diseases,” explained the co-investigator, Hélène Girouard.
“At the present time, surgery is the only way to treat patients with brain disorders. Moreover, while surgeons are able to operate to remove certain kinds of tumors, some disorders are located in the brain stem, amongst nerves, making surgery impossible,” added collaborator and senior author Anne-Sophie Carret.
Although the technology was developed using murine models and has not yet been tested in humans, the researchers are confident that future research will enable its use in people.
“Building on earlier findings and drawing on the global effort of an interdisciplinary team of researchers, this technology proposes a modern version of the vision described almost 40 years ago in the movie Fantastic Voyage, where a miniature submarine navigated in the vascular network to reach a specific region of the brain,” said principal investigator Sylvain Martel.
In earlier research, the team had managed to manipulate the movement of nanoparticles through the body using the magnetic forces generated by magnetic resonance imaging (MRI) machines.
To open the blood-brain barrier, the magnetic nanoparticles are sent to the surface of the blood-brain barrier at a desired location in the brain. Although it was not the technique used in this study, the placement could be achieved by using the MRI technology described above. Then, the researchers generated a radio-frequency field. The nanoparticles reacted to the radio-frequency field by dissipating heat thereby creating a mechanical stress on the barrier. This allows a temporary and localized opening of the barrier for diffusion of therapeutics into the brain.
The technique is unique in many ways as the researchers remarked.
“The result is quite significant since we showed in previous experiments that the same nanoparticles can also be used to navigate therapeutic agents in the vascular network using a clinical MRI scanner,” Martel remarked.
“Linking the navigation capability with these new results would allow therapeutics to be delivered directly to a specific site of the brain, potentially improving significantly the efficacy of the treatment while avoiding systemic circulation of toxic agents that affect healthy tissues and organs,” Carret added.
“While other techniques have been developed for delivering drugs to the blood-brain barrier, they either open it too wide, exposing the brain to great risks, or they are not precise enough, leading to scattering of the drugs and possible unwanted side effect,” Martel said.
Although there are many hurdles to overcome before the technology can be used to treat humans, the research team is optimistic.
“Although our current results are only proof of concept, we are on the way to achieving our goal of developing a local drug delivery mechanism that will be able to treat oncologic, psychiatric, neurological and neurodegenerative disorders, amongst others,” Carret concluded.
As mentioned, most drugs that show promise are stopped because the blood-brain barrier won’t let them pass. Even when those drugs do manage to get through, it is only minimal, this means more of the drug is used to get the desired effect. This means almost anything from painkillers to chemotherapy requires much larger doses than would be needed if the blood-brain barrier could be passed. The new research would not only help increase the number of drugs that are available to treat certain medical conditions, it means it could be done much cheaper than we can now.
Sources:
Tabatabaei, S., Girouard, H., Carret, A., & Martel, S. (2015). Remote control of the permeability of the blood–brain barrier by magnetic heating of nanoparticles: A proof of concept for brain drug delivery Journal of Controlled Release, 206, 49-57 DOI: 10.1016/j.jconrel.2015.02.027
What happens in the lab doesn't have to stay in the lab!
Related
This entry was posted on March 25, 2015 by The Lunatic. It was filed under Health and Medicine, Neuroscience Research and was tagged with blood-brain barrier, magnetic nanoparticles, medicine, neurology, peer reviewed, radio-frequency field, science, therapeutic molecules.
2 responses
But enough about us, what about you? Cancel reply
This site uses Akismet to reduce spam. Learn how your comment data is processed.



There was another paper published in Science Translational Medicine a few weeks ago that used microbubbles and focused ultrasound to break the blood brain barrier to deliver therapeutic agents to the brain. Here’s the link to the news story in Science: http://news.sciencemag.org/biology/2015/03/ultrasound-therapies-target-brain-cancers-and-alzheimer-s-disease
LikeLike
March 25, 2015 at 5:06 pm
Awesome, thanks for sharing that!
LikeLike
March 25, 2015 at 5:14 pm