Know your spinal cord – Somatosensory evoked potentials
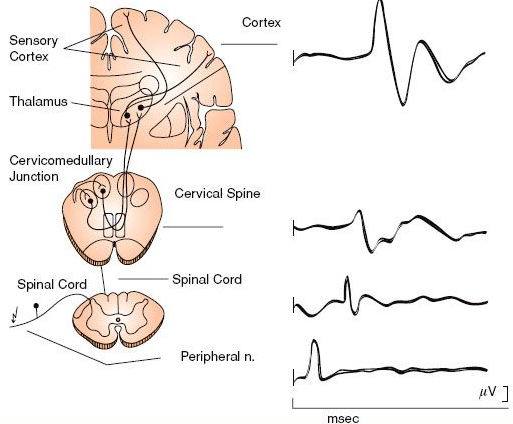
Somatosensory evoked potentials travel from peripheral nerves to the brain and we can record the response along the spinal cord and the brain non-invasively.
We’re back again with day forty-two of spinal cord knowledge series and day 200 in our 365 days of academia series! A friendly reminder that you can find each and every one of these posts in our very helpful neuroanatomy category. Yesterday we looked at motor evoked potentials, or electrical pulses that we create which travel from the brain to the muscles. Today we are looking at the almost reverse, signals we create originating in the peripheral nerves and arriving at the somatosensory cortex of the brain.
First a quick recap, we looked at the H-reflex, signals that travel from a peripheral nerve, to the spinal cord, and send a reflex response back to the corresponding muscles. We’ve seen the M-wave, which is just us stimulating the muscle (not necessarily intentionally). The F-wave was unique in that it forced a signal the wrong direction in a nerve, which stimulated the spinal cord circuitry causing it to rebound back down the same nerve. Finally, yesterday we looked at signals traveling from the brain/spinal cord to the muscles and we called those motor evoked potentials.
This means in our growing toolbox of things to probe the spinal cord, we have a handful of different ways to perturb the system and see what kind of response we get in return. However, most of these (all) start or end at the same place, the muscles. What we are missing is a tool to see how afferent signaling differs from efferent signaling. After all, what if the pathway is different, we could determine this using the latency going one direction and comparing it to the latency going in the other direction. That is where the somatosensory evoked potential comes into play.
The history of the somatosensory evoked potential (SEP) is surprisingly not that long. It was originally discovered in 1947. Later in the early 70’s and 80’s we also found that we could pick up the signal in the spinal cord as well as in subcortical regions of the brain (far field potentials) although there is (was) a lot of debate about the technique and what data it gave us, so it was not very widely used and has fallen out of favor for the most part. That isn’t to say that there aren’t researchers recording SEP’s from the spinal cord, we do. It’s just that the prognostic value of these results is not understood so it is mostly used for measuring latencies.
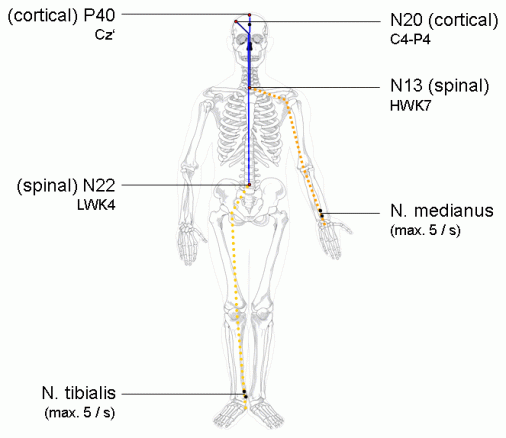
The associated response recorded from different locations on the spinal cord and brain when stimulating the tibial nerve and median nerve.
The image above shows how we stimulate peripheral nerves and the resulting wave they create when they reach the spinal cord or brain. NXX where XX is a number means that they find a negative (N) response XX milliseconds after the stimulus. So a N40 would be a negative potential recorded 40 milliseconds from the stimulus. Conversely a stimulus that creates a positive (P) response will be labeled PXX, where XX has the same meaning, the number of milliseconds from the stimulus to the recorded response. That means a P20 would be a positive potential recorded 20 milliseconds after the stimulus is applied.
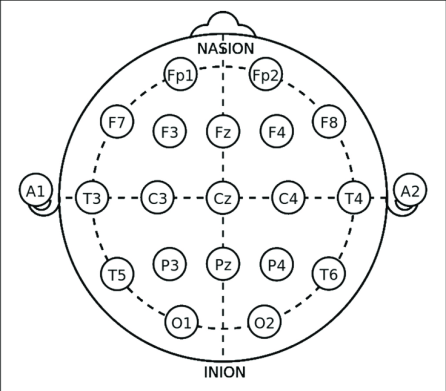
Cz (directly in the center) corresponds to the part of the brain responsible for foot/leg sensory processing while C4-P4 (right) is responsible for the left side of the body hand/arm sensory processing.
Cz is a specific location on the head that is defined by the 10-20 system (shown above) for EEG recording and corresponds to the location where we would see a response from the legs (the N. tibialis stimulus). C4-P4 corresponds to the location we would record a response from the hands (the N. medianus stimulus). For completeness, below is the somatosensory homunculus representation, which shows what body parts are associated with which portions of the somatosensory cortex, this way you can see why Cz is where we record for leg responses and C4-P4 is where we record for hand/arm responses.
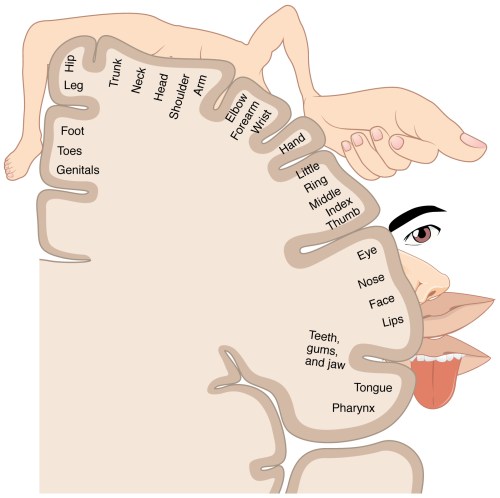
Half of the brain (mirrored to the other half) showing the somatosensory homunculus representation. Notice that the foot/leg are located in the medial portion, while the hand/arm are more laterally located. This makes it easier to determine right/left from the hands than legs because they are more spatially separate on the somatosensory cortex.
There are a lot of reasons to use SEPs, in my research we use them specifically to probe the spinal cord and they are used in combination with other stimuli, such as transcutaneous spinal cord stimulation, to determine the effect. There are also applications for this in surgery. When a surgeon is operating on the spinal cord for example, they can determine if the cord is still functioning using SEP’s without causing the person to involuntarily move. Below you can see what the SEP wave looks like as it travels through the body, this wave was created by stimulating the tibial nerve.
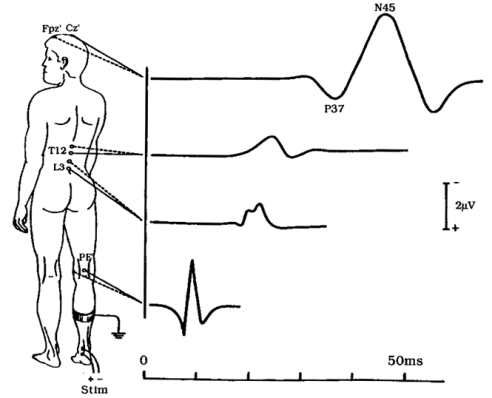
Tibial nerve SEP generating a distinct waveform at the spinal cord (L3, T12), and the brain (Cz) in the body
With that I think this is a good place to end our discussion on SEP’s and why they are useful and different from the other ways we stimulate. Next up I think we can get into one more tool we use called the V-wave (there are a lot of different ways to stimulate, as you can see). That will probably be the last of the electrophysiological introduction unless I am forgetting something (I am probably forgetting something).
Until next time, don’t stop learning!



But enough about us, what about you?