Know your spinal cord – Diastematomyelia
Diastematomyelia, a complicated name for a split spinal cord.
Day eighteen! Almost three weeks worth of fun spinal knowledge. For those tuning in, we have a neuroanatomy category just for these posts. Since we’ve covered most of the anatomy portion of the spinal cord, we’ve just started covering spinal disorders. If you’re here you’re probably wondering what diastematomyelia is, so let’s get started!
Diastematomyelia, a long name for a very rare spinal deformity. So we’ve talked quite a bit about how the body is controlled by the ipsilateral spinal cord. However, we also talked quite extensively about how certain tracts decussate IN the spinal cord. So when we talk about diastematomyelia we need to keep that bit of information in mind.
Now, diastematomyelia in the most basic sense is a split spinal cord. More interestingly this split happens longitudinally (in the sagittal plane or head to toe). The weird part about diastematomyelia is that it you might never notice that you have it. However, more often than not it is caught in childhood. Below is two different MRI scans showing what this split looks like from the coronal view and the transverse view


As you can see, the split is clearly visible and the characteristic butterfly shape of the grey matter is now more circular. The coronal view shows the typical location for this type of disorder, splitting usually occurs in the lumbar area of the cord. Interestingly cervical diastematomyelia is a very rare occurrence and we aren’t sure why this happens so we don’t understand why it is more prevalent in the lumbar area than the cervical.
From the image above we see the cord reattaches distally (below) to the split. This is the normal presentation, however there are cases where the cord does NOT reattach and that is called diplomyelia, which is a true duplication of the spinal cord.
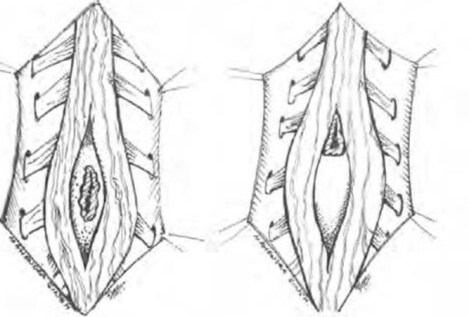
Symptoms of diastematomyelia are very similar to a tethered cord (see why we covered it in this order?) and over half of the cases of diastematomyelia also occur with a tethered cord. In most cases the cord is split by a bony spicule or a fibrous band and each half of the cord is encased in the dural sac individually. Below is a figure showing how the cord is split by a bony spicule (left) or by a band (right).
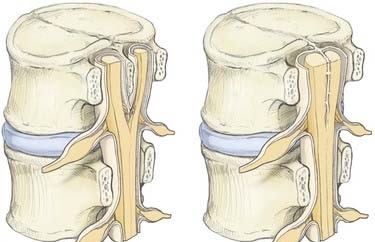
Spinal cord split by bony spicule (left) and fibrous band (right)
Typically surgery is indicated in this case, mostly to repair the bone spur (spicule) that causes the split and to repair any sort of tethering that occurs. When surgery is done, the duplication of the dural sac is often repaired since this can contribute to tethering as well.
That pretty much covers diastematomyelia! Thankfully like a tethered cord, it is very rare and is congenital so it’s not something you can develop as an adult (although symptoms can sometimes develop as an adult). Tomorrow we can talk spina bifida, that is a much more common condition unfortunately, but it is also complex with different presentations.
Until next time, don’t stop learning!



But enough about us, what about you?