Children could point the way to new HIV treatments

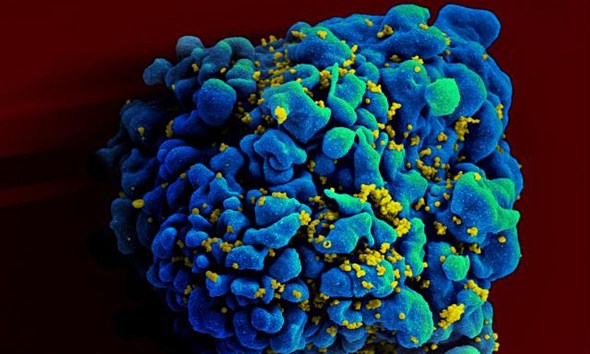
Children with HIV who can resist the disease progressing could point the way to new treatments for HIV infection that are more widely applicable to infected adults and children alike, an international team of researchers has found.
Tracking how HIV disrupts immune system informs vaccine development

One of the main mysteries confounding development of an HIV vaccine is why some people infected with the virus make the desired antibodies after several years, but a vaccine can’t seem to induce the same response.
Antibody therapy opens door to potential new treatment for HIV

The development of antiretroviral therapy, a combination of drugs that slows the replication of HIV in the body, has transformed the treatment of this infection. What was once a certain death sentence is now a chronic condition that people can live with for decades. But this therapy has drawbacks. There are side effects, including kidney problems, decreased bone density, and gastrointestinal problems. And if a person discontinues his or her treatment, even missing a few doses, the level of the virus in the body is able to rebound quickly.
Neurological adaptations to the presence of toxic HIV protein
Nearly half of HIV infected patients suffer from impaired neurocognitive function. The HIV protein transactivator of transcription (Tat) is an important contributor to HIV neuropathogenesis because it is a potent neurotoxin that continues to be produced despite treatment with antiretroviral therapy.
Closing the loop on an HIV escape mechanism
Nearly 37 million people worldwide are living with HIV. When the virus destroys so many immune cells that the body can’t fight off infection, AIDS will develop. The disease took the lives of more than a million people last year.
An antibody that can attack HIV in new ways
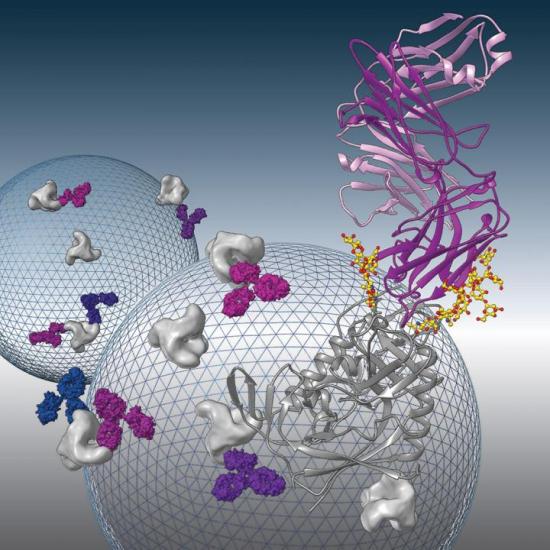
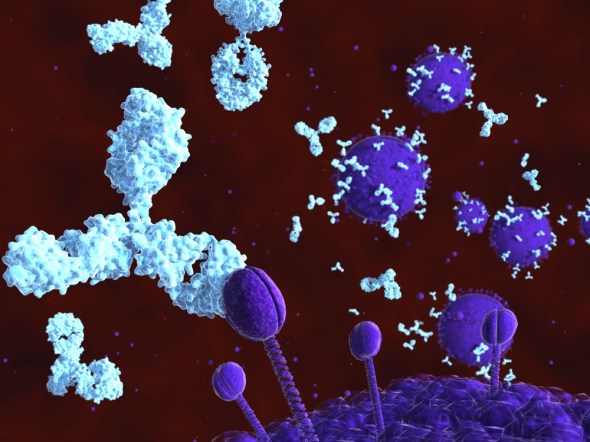
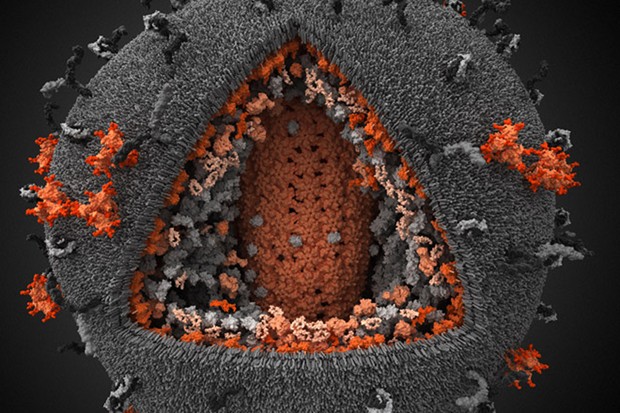
Broadly neutralizing antibodies to HIV-1 envelope glycoprotein are being evaluated as therapeutics to prevent or treat HIV-1 infection. Structural analysis of one such antibody, 8ANC195, revealed a new conformation of the envelope protein. The image shows the X-ray crystal structure of 8ANC195 in complex with the gp120 subunit of the envelope protein. The background shows schematic representations of HIV-1 virus particles studded with envelope proteins being recognized by 8ANC195 antibodies.
Image credit goes to: Louise Scharf/Caltech
Proteins called broadly neutralizing antibodies (bNAbs) are a promising key to the prevention of infection by HIV, the virus that causes AIDS. bNAbs have been found in blood samples from some HIV patients whose immune systems can naturally control the infection. These antibodies may protect a patient’s healthy cells by recognizing a protein called the envelope spike, present on the surface of all HIV strains and inhibiting, or neutralizing, the effects of the virus. Now Caltech researchers have discovered that one particular bNAb may be able to recognize this signature protein, even as it takes on different conformations during infection–making it easier to detect and neutralize the viruses in an infected patient.
HIV particles do not cause AIDS, our own immune cells do
Researchers have revealed that HIV does not cause AIDS by the virus’s direct effect on the host’s immune cells, but rather through the cells’ lethal influence on one another. HIV can either be spread through free-floating virus that directly infect the host immune cells or an infected cell can pass the virus to an uninfected cell.
How long have primates been infected with viruses related to HIV?
Disease-causing viruses engage their hosts in ongoing arms races: positive selection for antiviral genes increases host fitness and survival, and viruses in turn select for mutations that counteract the antiviral host factors. Studying such adaptive mutations can provide insights into the distant history of host-virus interactions. A study of antiviral gene sequences in African monkeys suggests that lentiviruses closely related to HIV have infected primates in Africa as far back as 16 million years.
Research advances potential for test and vaccine for genital and oral herpes
Findings from a pair of new studies could speed up the development of a universally accurate diagnostic test for human herpes simplex viruses (HSV), according to researchers at Johns Hopkins and Harvard universities and the National Institutes of Health (NIH). The work may also lead to the development of a vaccine that protects against the virus.
Some vaccines support evolution of more-virulent viruses

This image shows chickens in agricultural production. Image credit goes to: Andrew Read, Penn State University
Scientific experiments with the herpes virus such as the one that causes Marek’s disease in poultry have confirmed, for the first time, the highly controversial theory that some vaccines could allow more-virulent versions of a virus to survive, putting unvaccinated individuals at greater risk of severe illness. The research has important implications for food-chain security and food-chain economics, as well as for other diseases that affect humans and agricultural animals.
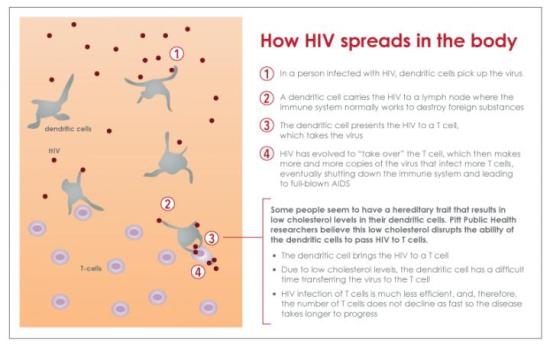
Cholesterol metabolism in immune cells linked to HIV progression, may lead to new therapy
Enhanced cholesterol metabolism in certain immune cells may help some people infected with HIV naturally control disease progression, according to new research. The findings provide a basis for potential development of new approaches to control HIV infection by regulating cellular cholesterol metabolism.
The health effects of homophobia
Homophobia, since people are (finally) stigmatizing racism, it’s just another excuse to be able to treat people who are slightly different like they are garbage. To that end, I have bad news for gay and bisexual men living in European countries. The ones with strong attitudes and policies against homosexuality are far less likely to use HIV-prevention services, test for HIV, and discuss their sexuality with health providers, according to research led by Yale School of Public Health (YSPH).
First human HIV-antibody trials, results are promising
While there is no cure for HIV, a select few known as HIV controllers can literally live with it. Over the years work has been done trying to figure out what makes these individuals so special and it has helped researchers in the fight against HIV. While we are still searching for a vaccine, researchers have now found that a single infusion of an experimental anti-HIV antibody called 3BNC117 resulted in significantly decreased HIV levels that persisted for as long as 28 days in HIV-infected individuals, according to Phase 1 clinical trial findings.
Scientists find anti-HIV agent and possible start for a vaccine
We may just have found a missing link in the fight towards an HIV vaccine. No, this is not an over-hyped headline, in a remarkable new advance against the virus that causes AIDS, scientists have announced the creation of a novel drug candidate that is so potent and universally effective, it might work as part of an unconventional vaccine.
Researchers discover viral ‘Enigma machine’
Antibiotics are for infections, vaccines are for viruses, and unfortunately both bacteria AND viruses mutate. So when someone has AIDS for example it is hard to fight since a vaccine would be hard to produce given how rapidly it evolves. Well now researchers may be one step closer to solving the problem since they have cracked a code that governs infections by a major group of viruses which includes the common cold and polio.
HIV vaccines may make things worse
Despite what conspiracy theorists say, there is no cure for HIV. Not that people aren’t feverously working hard to find one, it is just really hard to do. To illustrate that point researchers have found that vaccines designed to protect against HIV can backfire and lead to increased rates of infection. This unfortunate effect has been seen in more than one vaccine clinical trial.
Hiding cells to prevent HIV transmission
The fight against HIV is ongoing and despite our rapid progression against the disease we still lack a cure or even adequate treatment for people infected. However, new research suggests that cloaking immune cells with antibodies that block T cell trafficking to the gut can substantially reduce the risk of viral transmission, at least in a non-human primate model of HIV infection. If it works out, this could help slow down the spread of HIV and give people a better shot at a normal life.
A Possible Genetic “Cure” for HIV… Maybe
Let’s face it, a cure for HIV probably won’t be coming around for awhile. That slippery little virus manages to avoid everything we throw at it. Well researchers at Massachusetts General (MGH) and Boston Children’s hospitals (BCH) tried to take another crack at the problem. For the first time they have used a relatively new gene-editing technique to create what could prove to be an effective technique for blocking HIV from invading and destroying patients’ immune systems.
Where HIV hides
HIV is hard to get rid of,not because it primarily resides in the blood, but because of where it hides when antiretrovirals drop HIV levels. So the real question is where does HIV hide? Unfortunately those antiretroviral drugs can usually control the virus, but can’t completely eliminate it. So any strategy to eradicate HIV from the body has to take into account not only the main group of immune cells the virus targets, called CD4 or helper T cells, but other infected cells as well.
Bringing the Fight to hidden HIV
We’ve got even more news for the HIV cure front. Yesterday we talked about broadly neutralizing antibodies, today we are going to be touching on that yet again,so if you missed it, you can read more about that here. Now, although HIV can now be effectively suppressed using anti-retroviral drugs, it still comes surging back the moment the flow of drugs is stopped. We sadly saw this delayed response in an infant that was thought to be effectively “cured” of HIV. It is unfortunate, but latent reservoirs of HIV-infected cells, invisible to the body’s immune system and unreachable by pharmaceuticals, ensure that the infection will rebound after therapy is terminated. This is a big reason that, even when the viral load drops below detection, you still need constant check ups and continuous anti-retrovirals.
HIV Vaccine One Step Closer to Reality
The war on HIV, that tricky little guy has avoided every thing we could throw at it in a broad sense. Sure a few people here and there get lucky, but we have yet to actually make any sort of we’re going to kick your ass headway [don’t worry it’s the technical term for it]. That is hopefully going to change with a new scientific discovery that has enormous implications for HIV vaccine development. Researchers have uncovered novel properties of special HIV antibodies that promise to help eliminate HIV.
Antiretrovirals and Pregnancy Risk
Don’t drink when you are pregnant, we all know that you aren’t supposed to do that. We also know you shouldn’t smoke, use drugs, and should talk to your Doctor about what medications you are taking while pregnant. So then what about when your husband is HIV positive and you want to get pregnant, are antiretrovirals safe to be using while a woman is pregnant? As it turns out, there is no real research on it, and the answer might be a little harder to get at.
A New way to Fight HIV, Using your Genome!

Outsmarting something as “simple” as a virus doesn’t seem like much of a challenge. If only you could set it down to take the SAT’s or something. Unfortunately, in the body fighting HIV is more like guerrilla warfare, you take the big losses for a small win. This is no way to wage a war, but HIV is smart. It mutates and sidesteps anything we’ve been able to throw at it. We don’t have a cure, or a vaccine, but we do have scientists trying. However, new research has made a crucial jump to throwing a curveball at HIV and with it, a possible cure.