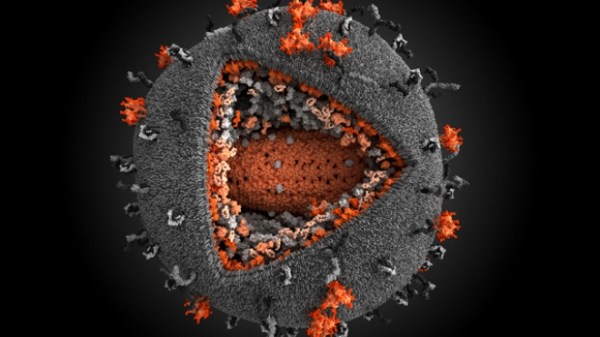
Tracking how HIV disrupts immune system informs vaccine development

One of the main mysteries confounding development of an HIV vaccine is why some people infected with the virus make the desired antibodies after several years, but a vaccine can’t seem to induce the same response.
Experimental antibiotic treats deadly MRSA infection

The antibiotic arms race is on, while we are rushing to find new antibiotics, bacteria are working on finding ways around them. With that in mind, a new experimental antibiotic developed by a team of scientists successfully treats the deadly MRSA infection and restores the efficacy of a commonly prescribed antibiotic that has become ineffective against MRSA.
Zika virus directly infects brain cells and evades immune system detection

The mosquito-borne Zika virus linked to microcephaly and other neurological problems in newborns of affected mothers directly infects the brain progenitor cells destined to become neurons. The team of researchers used a strain of Zika currently impacting the Americas, and found that the virus infects about 20 percent of cells on average, evades immune system detection, and continues to replicate for weeks.
Antibody therapy opens door to potential new treatment for HIV

The development of antiretroviral therapy, a combination of drugs that slows the replication of HIV in the body, has transformed the treatment of this infection. What was once a certain death sentence is now a chronic condition that people can live with for decades. But this therapy has drawbacks. There are side effects, including kidney problems, decreased bone density, and gastrointestinal problems. And if a person discontinues his or her treatment, even missing a few doses, the level of the virus in the body is able to rebound quickly.
Scientific evidence of sexual transmission of the Zika virus

Well, we know now that ZIKA causes microcephaly, at least that is the latest findings. Things don’t look so good on other ZIKA fronts either, a new study confirms that the virus can be transmitted sexually. The analyses have shown 100% genetic correlation between the form of the virus present in a man who contracted the virus in Brazil and that of a woman who had never travelled in the epidemic area, but who had sexual relations with him.
Road rage and toxoplasmosis: Return of the parasite

It was a clear case of a false alarm, toxoplasmosis, a parasite that infects mice and cats was thought to have an effect on humans. However, after a thorough review of the data it was off the hook, or so we thought. Individuals with a psychiatric disorder involving recurrent bouts of extreme, impulsive anger–road rage, for example–are more than twice as likely to have been exposed to a common parasite than healthy individuals with no psychiatric diagnosis.
Viruses ‘piggyback’ on hosts success

In the microscopic life that thrives around coral reefs, researchers have discovered an interplay between viruses and microbes that defies conventional wisdom. As the density of microbes rises in an ecosystem, the number of viruses infecting those microbes rises with it. It has generally been assumed that this growing population of viruses, in turn, kills more and more microbes, keeping the microbial population in check. It’s a model known as “kill-the-winner” — the winners being the blooming microbial cells and the killers being the viruses (mostly bacteria-killing viruses known as bacteriophages) that infect them.
Preemies’ gut bacteria reveal vast scope of antibiotic resistance

Yesterday we blogged about the emergent and increasing antibiotic resistance problem, which was good — or bad timing — depending on how you look at it. A new study of gut bacteria in premature infants reveals the vast scope of the problem of antibiotic resistance and gives new insight into the extreme vulnerability of these young patients, according to researchers.
Antibiotic resistance, evolution, and our future

Without the discovery of antibiotics we could not — and most certainly would not — be living in the world we do today. It was a discovery that would save countless lives, while simultaneously compromising our future. From the use (and unfortunate misuse) of antibiotics, we gave rise to more virulent bacteria that have become resistant to more and more types of antibiotics.
Zika virus infects human neural stem cells, but…

The Zika virus infects a type of neural stem cell that gives rise to the brain’s cerebral cortex, Johns Hopkins and Florida State researchers have found. On laboratory dishes, these stem cells were found to be havens for viral reproduction, resulting in cell death and/or disruption of cell growth. While this study does not prove the direct link between Zika and microcephaly, it does pinpoint where the virus may be doing the most damage.
Scientists discover the way to a new generation of antibiotics

Antibiotic resistance is becoming a common occurrence. Once isolated, more and more we are turning away from the traditional antibiotics to our so called “last line of defense” antibiotics to fight infections. Sadly, in a growing number of cases these antibiotics are having less of an effect. However, new research reveals the mechanism by which drug-resistant bacterial cells maintain a defensive barrier.
Neurological adaptations to the presence of toxic HIV protein
Nearly half of HIV infected patients suffer from impaired neurocognitive function. The HIV protein transactivator of transcription (Tat) is an important contributor to HIV neuropathogenesis because it is a potent neurotoxin that continues to be produced despite treatment with antiretroviral therapy.
Neurons in your gut help the immune system keep inflammation in check

The immune system exercises constant vigilance to protect the body from external threats–including what we eat and drink. A careful balancing act plays out as digested food travels through the intestine. Immune cells must remain alert to protect against harmful pathogens like Salmonella, but their activity also needs to be tempered since an overreaction can lead to too much inflammation and permanent tissue damage.
Seeing viruses in a new light

Want to make a virus? It’s easy: combine one molecule of genomic nucleic acid, either DNA or RNA, and a handful of proteins, shake, and in a fraction of a second you’ll have a fully-formed virus. While that may sound like the worst infomercial ever, in many cases making a virus really is that simple. Viruses such as influenza spread so effectively, and as a result can be so deadly to their hosts, because of their ability to spontaneously self-assemble in large numbers.
Certain herpes viruses can infect human neurons

For years, researchers have noted a tantalizing link between some neurologic conditions and certain species of the herpes virus. In patients with Alzheimer’s disease, multiple sclerosis, and cerebellar ataxia, among other neuropathies, the cerebrospinal fluid teems with Epstein-Barr virus (EBV). Yet, the nature of that link has remained unclear, as it has been assumed that EBV, as well as other viruses in the same sub-family, called gammaherpesviruses, cannot infect neurons.
Closing the loop on an HIV escape mechanism
Nearly 37 million people worldwide are living with HIV. When the virus destroys so many immune cells that the body can’t fight off infection, AIDS will develop. The disease took the lives of more than a million people last year.
The mysterious fungus that has major health consequences

Researchers at the University of Toronto examined fungi in the mucus of patients with cystic fibrosis and discovered how one particularly cunning fungal species has evolved to defend itself against neighbouring bacteria. A regular resident of our microbiome – and especially ubiquitous in the lungs of cystic fibrosis patients -the Candida albicans fungus is an “opportunistic pathogen.”
The first line of defense? Think Mucus
By licking a wound it heals faster — this is not simply popular belief, but scientifically proven. Our saliva consists of water and mucus, among other things, and the mucus plays an important role. It stimulates white blood cells to build a good defense against invaders, according to a group of researchers at Lund University in Sweden together with colleagues from Copenhagen and Odense in Denmark.
Predicting what side effects you’ll experience from a drug
Researchers at the University of California, San Diego have developed a model that could be used to predict a drug’s side effects on different patients. The proof of concept study is aimed at determining how different individuals will respond to a drug treatment and could help assess whether a drug is suitable for a particular patient based on measurements taken from the patient’s blood.
What blocks pro-vaccine beliefs?
Despite rhetoric that pits “anti-vaxxers” versus “pro-vaxxers,” most new parents probably qualify as vaccine-neutral–that is, they passively accept rather than actively demand vaccination. Unless there is an active threat of polio or whooping cough, they have to remind themselves that injecting their crying infant with disease antigens is a good thing.
Intestinal worms ‘talk’ to gut bacteria to boost immune system
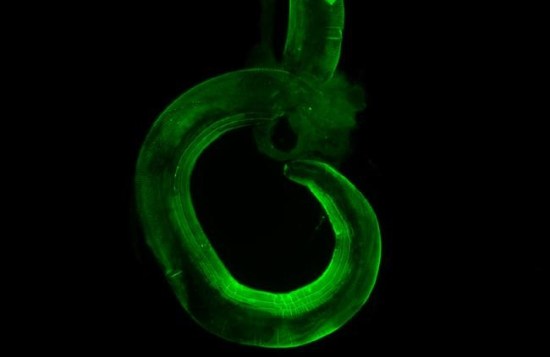
This is the helminth Heligmosomoides polygyrus bakeri (Hpb), which infects rodents. Here seen under fluorescent staining. Hpb was used in the mouse part of this study.
Image credit goes to: Nicola Harris/EPFL
When you think parasites you probably don’t think of anything helpful. However, this isn’t the case and certain parasites inadvertently help the host by helping themselves. In fact, researchers have discovered how intestinal worm infections cross-talk with gut bacteria to help the immune system.
Decontaminating infant formula with the bacteriophage
When dealing with bacteria, antibiotics are usually the frontrunner, but there are cases where antibiotics are a big no. Take baby formula for instance, we cannot use antibiotics to keep bacteria at bay. This has posed a safety problem in recent years, but researchers have shown that we can use a natural enemy of bacteria to fight back without risk to infants’ health.
How plants turn into zombies
It begins as a fairy tale which later turns into a horror story: Lusciously flowering plants, surrounded by a large number of insects. Usually, both sides profit from the encounter: Feasting on the plant juice and pollen, the insects pollinate the flowers and thus secure the survival of the plants. However, sometimes the insects – in this case a certain species of leafhoppers – can bring disaster to the plants, which they are not able to overcome.
It’s alive!! Study adds to evidence that viruses are alive

The diverse physical attributes, genome sizes and lifestyles of viruses make them difficult to classify. A new study uses protein folds as evidence that viruses are living entities that belong on their own branch of the tree of life.
Image credit goes to: Julie McMahon
Classifying something as living isn’t as easy as it sounds, after all we are all atoms, so when do atoms go from nonliving to living? Despite the complexities of viruses, we have historically deemed them nonliving. However, a new analysis supports the hypothesis that viruses are living entities that share a long evolutionary history with cells. The study offers the first reliable method for tracing viral evolution back to a time when neither viruses nor cells existed in the forms recognized today.
Viruses flourish in guts of healthy babies
Bacteria aren’t the only nonhuman invaders to colonize the gut shortly after a baby’s birth. Viruses also set up house there, according to new research at Washington University School of Medicine in St. Louis. All together, these invisible residents are thought to play important roles in human health.
HIV particles do not cause AIDS, our own immune cells do
Researchers have revealed that HIV does not cause AIDS by the virus’s direct effect on the host’s immune cells, but rather through the cells’ lethal influence on one another. HIV can either be spread through free-floating virus that directly infect the host immune cells or an infected cell can pass the virus to an uninfected cell.
How long have primates been infected with viruses related to HIV?
Disease-causing viruses engage their hosts in ongoing arms races: positive selection for antiviral genes increases host fitness and survival, and viruses in turn select for mutations that counteract the antiviral host factors. Studying such adaptive mutations can provide insights into the distant history of host-virus interactions. A study of antiviral gene sequences in African monkeys suggests that lentiviruses closely related to HIV have infected primates in Africa as far back as 16 million years.
Research advances potential for test and vaccine for genital and oral herpes
Findings from a pair of new studies could speed up the development of a universally accurate diagnostic test for human herpes simplex viruses (HSV), according to researchers at Johns Hopkins and Harvard universities and the National Institutes of Health (NIH). The work may also lead to the development of a vaccine that protects against the virus.
New approach for making vaccines for deadly diseases
Researchers have devised an entirely new approach to vaccines – creating immunity without vaccination. The team has demonstrated that animals injected with synthetic DNA engineered to encode a specific neutralizing antibody against the dengue virus were capable of producing the exact antibodies necessary to protect against disease, without the need for standard antigen-based vaccination. Importantly, this approach, termed DMAb, was rapid, protecting animals within a week of administration.
Some vaccines support evolution of more-virulent viruses

This image shows chickens in agricultural production. Image credit goes to: Andrew Read, Penn State University
Scientific experiments with the herpes virus such as the one that causes Marek’s disease in poultry have confirmed, for the first time, the highly controversial theory that some vaccines could allow more-virulent versions of a virus to survive, putting unvaccinated individuals at greater risk of severe illness. The research has important implications for food-chain security and food-chain economics, as well as for other diseases that affect humans and agricultural animals.
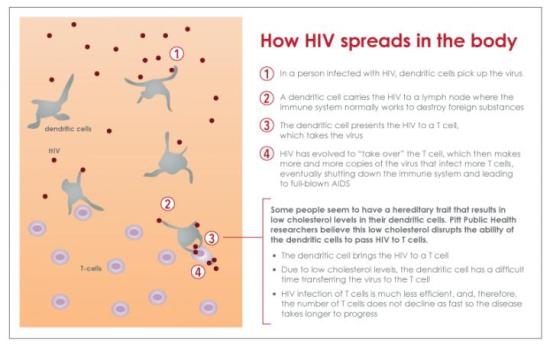
Cholesterol metabolism in immune cells linked to HIV progression, may lead to new therapy
Enhanced cholesterol metabolism in certain immune cells may help some people infected with HIV naturally control disease progression, according to new research. The findings provide a basis for potential development of new approaches to control HIV infection by regulating cellular cholesterol metabolism.
Discovery points to a new path toward a universal flu vaccine
Flu vaccines can be something of a shot in the dark. Not only must they be given yearly, there’s no guarantee the strains against which they protect will be the ones circulating once the season arrives. New research by Rockefeller University scientists suggests it may be possible to harness a previously unknown mechanism within the immune system to create more effective and efficient vaccines against this ever-mutating virus.
A single mutation helped last year’s flu virus gain an advantage over the vaccine
The 2014-2015 flu vaccine didn’t work as well compared to previous years because the H3N2 virus recently acquired a mutation that concealed the infection from the immune system. A new study reveals the major viral mutation responsible for the mismatch between the vaccine strain and circulating strains. The research will help guide the selection of viral strains for future seasonal flu vaccines.
First functional, synthetic immune organ with controllable antibodies created by engineers
Cornell University engineers have created a functional, synthetic immune organ that produces antibodies and can be controlled in the lab, completely separate from a living organism. The engineered organ has implications for everything from rapid production of immune therapies to new frontiers in cancer or infectious disease research.
The health effects of homophobia
Homophobia, since people are (finally) stigmatizing racism, it’s just another excuse to be able to treat people who are slightly different like they are garbage. To that end, I have bad news for gay and bisexual men living in European countries. The ones with strong attitudes and policies against homosexuality are far less likely to use HIV-prevention services, test for HIV, and discuss their sexuality with health providers, according to research led by Yale School of Public Health (YSPH).
First human HIV-antibody trials, results are promising
While there is no cure for HIV, a select few known as HIV controllers can literally live with it. Over the years work has been done trying to figure out what makes these individuals so special and it has helped researchers in the fight against HIV. While we are still searching for a vaccine, researchers have now found that a single infusion of an experimental anti-HIV antibody called 3BNC117 resulted in significantly decreased HIV levels that persisted for as long as 28 days in HIV-infected individuals, according to Phase 1 clinical trial findings.
Smoking, bad for you, good for MRSA
Methicillin-resistant Staphylococcus aureus (MRSA), an antibiotic-resistant superbug, can cause life-threatening skin, bloodstream and surgical site infections or pneumonia. It has been a tough battle finding ways to fight it and research now shows, cigarette smoke may make matters worse. The study shows that MRSA bacteria exposed to cigarette smoke become even more resistant to killing by the immune system.