And nothing was wrong with me…

Last summer I had some sort of autoimmune thing kick up. Frankly I’m not sure it was autoimmune or what the hell it was, but it hurt, left me feeling exhausted, and caused my hands, face, and elbows to form raised red spots that later peeled off (here). It was incredibly painful, made me question the minor breakouts of whatever it was that had been going on for a good ten years or so prior, and was a red flag that I was not okay. But the pandemic has been ongoing so getting attention from the VA, which is notoriously awful, had been difficult. Had been, I finally got the chance to see someone.
(more…)Day 347: The precipice of … something


Today is a mash of things, because frankly I still am not feeling good. My the scaly bits on my hands, face, and apparently elbows (missed that one until last night) haven’t gotten worse (yay), but they haven’t gotten better either (boo). On one hand it’s a realization that whatever is wrong with me was worse than I had thought, on the other, the world still moves forward and unfortunately I have work to do, so what’s a guy to do?
Day 346: What is going on with me?


It’s going to sound like depression. I realize that as we dive into today. I don’t normally do this, but I’m rewriting this intro because I know what it sounds like. It’s not that, this is something else and it worries me. I know depression, I’m good friends with depression, this is something different so don’t tell me it’s depression, it’s not I promise. It just happens to be worse than I can ever remember right as I’m dealing with the worst flare up [of whatever I have going on] in my entire life, so it couldn’t be a coincidence … could it?
Omega-3 fatty acid stops known trigger of lupus

A team of researchers has found that consuming an omega-3 fatty acid called DHA, or docosahexaenoic acid, can stop a known trigger of lupus and potentially other autoimmune disorders. DHA can be found in fatty, cold-water fish and is produced by the algae that fish eat and store in their bodies. It can be found in fish oil supplements as well, used by more than 30 million Americans.
Children could point the way to new HIV treatments

Children with HIV who can resist the disease progressing could point the way to new treatments for HIV infection that are more widely applicable to infected adults and children alike, an international team of researchers has found.
Tracking how HIV disrupts immune system informs vaccine development

One of the main mysteries confounding development of an HIV vaccine is why some people infected with the virus make the desired antibodies after several years, but a vaccine can’t seem to induce the same response.
Celiac disease: ‘Junk’ DNA not quite junk

Despite the fad to go ‘gluten free,’ the only people who actually suffer from consumption of gluten are those with coeliac disease — so if you don’t have the disease and like to limit yourself to gluten-free foods, you are missing out, and no gluten intolerance is not a real thing. The problem comes from the immune system and is manifested as intolerance to gluten — tasty proteins present in wheat, rye, and barley that help give baked goods their fluff. The intolerance leads to an inflammatory reaction in the small intestine that hampers the absorption of nutrients.
Using precision medicine to define the genetics of autoimmune disease

Demonstrating the potential of precision medicine, an international study used next-generation DNA sequencing technology to identify more than 1,000 gene variants that affect susceptibility to systemic lupus erythematosus (SLE). Precision medicine is an emerging field that aims to deliver highly personalized health care by understanding how individual differences in genetics, environment, and lifestyle impact health and disease.
Does your immune system play a larger role in Alzheimer’s disease than thought?

Immune cells that normally help us fight off bacterial and viral infections may play a far greater role in Alzheimer’s disease than originally thought, according to University of California, Irvine neurobiologists with the Sue & Bill Gross Stem Cell Research Center and the Institute for Memory Impairments and Neurological Disorders.
Novel insights into genetic cause of autoimmune diseases
A collaboration between researchers at the Babraham Institute and the University of Manchester has mapped the physical connections occurring in the genome to shed light on the parts of the genome involved in autoimmune diseases. Using a new technique, called Capture Hi-C, the team revealed novel insights into how changes in the genetic sequence have a biological effect and increase the risk of disease.
Master switch for brain development
Scientists at the Institute of Molecular Biology (IMB) in Mainz have unraveled a complex regulatory mechanism that explains how a single gene can drive the formation of brain cells. The research is an important step towards a better understanding of how the brain develops. It also harbors potential for regenerative medicine.
Connecting Alzheimer’s disease and the immune system
The role of the immune system in Alzheimer’s disease is a hot topic, but exactly how the two are connected and what interventions could help lower risk remain a mystery. In a new study, researchers in the Ann Romney Center for Neurologic Diseases at Brigham and Women’s Hospital (BWH) investigate how genetic risk factors for Alzheimer’s disease may influence a key type of immune cell. Their results lay the groundwork for designing better therapeutic strategies and better prediction tools for risk of developing Alzheimer’s disease.
Immune system may be pathway between nature and good health
Research has found evidence that spending time in nature provides protections against a startling range of diseases, including depression, diabetes, obesity, ADHD, cardiovascular disease, cancer, and many more. How this exposure to green space leads to better health has remained a mystery. After reviewing hundreds of studies examining nature’s effects on health, researchers believe the answer lies in nature’s ability to enhance the functioning of the body’s immune system.
Study details ‘rotten egg’ gas’ role in autoimmune disease
The immune system not only responds to infections and other potentially problematic abnormalities in the body, it also contains a built-in brake in the form of regulatory T cells, or Tregs. Tregs ensure that inflammatory responses don’t get out of hand and do damage. In autoimmune diseases, sometimes these Treg cells don’t act as they should.
Childhood cancer cells drain immune system’s batteries
Cancer cells in neuroblastoma contain a molecule that breaks down a key energy source for the body’s immune cells, leaving them too physically drained to fight the disease, according to new research. Cancer Research UK-funded scientists have discovered that the cells in neuroblastoma – a rare type of childhood cancer that affects nerve cells – produce a molecule that breaks down arginine, one of the building blocks of proteins and an essential energy source for immune cells.
Study shows long-term effects of type 2 diabetes on the brain, thinking
In just two years, people with type 2 diabetes experienced negative changes in their ability to regulate blood flow in the brain, which was associated with lower scores on tests of cognition skills and their ability to perform their daily activities, according to a new study.
Link between autoimmune diseases, medications, and a dangerous heart condition
Image credit goes to: The one and only Beatrice the biologist
Mohamed Boutjdir, PhD, professor of medicine, cell biology, and physiology and pharmacology at SUNY Downstate Medical Center, has led a study with international collaborators identifying the mechanism by which patients with various autoimmune and connective tissue disorders may be at risk for life-threatening cardiac events if they take certain anti-histamine or anti-depressant medications. Dr. Boutjdir is also director of the Cardiac Research Program at VA New York Harbor Healthcare System.
Autoimmunity: New immunoregulation and biomarker
Clinicians at Ludwig-Maximilians-Universitaet (LMU) in Munich have elucidated a mechanism involved in determining the lifespan of antibody-producing cells, and identified a promising new biomarker for monitoring autoimmune diseases like multiple sclerosis and lupus erythematosus.
New drug can clear all psoriasis symptoms
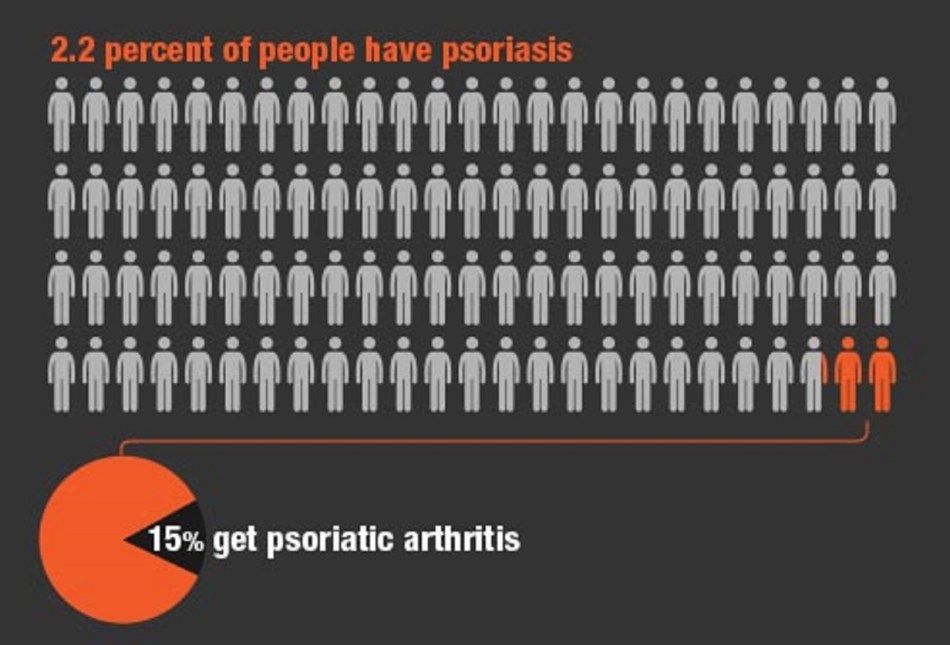
Good news for anyone who has psoriasis, a University of Manchester led trial of a new drug has resulted in 40 percent of people showing a complete clearance of psoriatic plaques after 12 weeks of treatment and over 90 percent showing improvement. The research tested 2,500 people with psoriasis. Half were given a new drug – ixekizumab – either once every two or four weeks. The other half were given a placebo or a widely used drug for psoriasis called etanercept.
First functional, synthetic immune organ with controllable antibodies created by engineers
Cornell University engineers have created a functional, synthetic immune organ that produces antibodies and can be controlled in the lab, completely separate from a living organism. The engineered organ has implications for everything from rapid production of immune therapies to new frontiers in cancer or infectious disease research.
Researchers find genetic link between overactive and underactive immune systems
In the largest genetic study to date of a challenging immunodeficiency disorder, scientists have identified a gene that may be a “missing link” between overactive and underactive immune activity. The gene candidate also plays a key role in autoimmune diseases such as type 1 diabetes, rheumatoid arthritis and even allergies.
Enzyme in cosmetic products can cause allergy
Papain is found naturally in papaya and is often referred to as a “plant-based pepsin” in reference to the digestive enzyme pepsin that is present in the stomach. Researchers looked at the effect of papain directly on the skin of mice as well as on skin cells in the petri dish. Skin consists of several layers joined via cellular connections called “tight junctions”. The project team showed that papain induces a breakdown of these cell-cell junctions. On the skin, papain results in a loss of the barrier function.
Antibody therapy offers possible cure for psoriasis
Sure it’s not sexy, you probably won’t be asked for donations towards a cure, or to run/walk/dive for awareness, and it probably won’t kill you. Psoriasis is an autoimmune disease, but chances are you are not familiar with it. It causes red, scale-like patches, sometimes covering a majority of the body. It’s itchy, painful, and embarrassing (to put it nicely). I know first hand as I suffer from it albeit mildly. I say mildly since I am lucky the patches are fairly small, but not so lucky for me they pop up on my face, often. However, new research is offering hope for anyone suffering from psoriasis and possibly a cure.
Alzheimer’s, the autoimmune disease?
Brain levels of the lipid ceramide are high in Alzheimer’s disease, and now scientists have found increased levels of an antibody to the lipid in their disease model. While some members of this lipid family are a plus in skin cream, inside the brain, ceramide appears to increase beta amyloid production and help the iconic plaque kill brain cells in Alzheimer’s.
Not “just” crazy – Some psychoses caused by autoimmunity
Antibodies defend the body against bacterial, viral, and other invaders. But sometimes the body makes antibodies that attack healthy cells. In these cases, autoimmune disorders develop. Immune abnormalities in patients with psychosis have been recognized for over a century, but it has been only relatively recently that scientists have identified specific immune mechanisms that seem to directly produce symptoms of psychosis, including hallucinations and delusions. In other words, some forms of psychoses might just be an autoimmune disorder.
New compounds protect nerves from the damage of MS
Autoimmune diseases are tough to live with, frankly we don’t really understand the reasons they start at all, how to treat them, or even where to start in forming a cure. Well there might be some good news — as far as a treatment goes anyway — a newly characterized group of pharmacological compounds block both the inflammation and nerve cell damage seen in mouse models of multiple sclerosis.
A New Discovery in the Treatment of Autoimmunity and Chronic Inflammation
Lupus, Type 1 diabetes, and multiple sclerosis are all diseases brought on by autoimmunity — the bodies inability to tell itself apart from foreign invaders. Finding a cure, or even a suitable treatment has been to put it gently a long, painful road, with little to show for it. On the forefront of the war against the body betrayal is immunosuppressants, which with them carry their own set of side effects and in most cases only off mild to moderate relief of symptoms. But that is all changing and new research on something called immunoproteasomes offer that new hope.
Nanosponges Clean up Antibody-mediated Autoimmune Disease
What does lupus, rheumatoid arthritis, type I diabetes, multiple sclerosis, and rheumatic heart disease have in common? All of these (and many other) apparently unrelated disorders are caused by autoimmunity, in which the immune system produces antibodies that attack normal, healthy cells and tissues. Currently considered incurable, these autoimmune diseases can be managed, but to varying degrees and not without serious side effects. Moreover, autoimmune diseases include a wide range of dysfunctional immune responses known as type II, type III, and type IV immune hypersensitivity reactions.
New Hope for Autoimmune Diseases
Autoimmune diseases are on the rise. Since I have a history of over sharing, my Uncle suffered from a form of lupus. It caused him intense and — in my opinion — unbearable pain although he shouldered it like the incredible man he was and never complained. My sister unfortunately is suffering from a rare disease that has yet to be diagnosed, which in my opinion has autoimmune dysfunction as the root cause. If you or anyone you know suffers in a similar fashion then you know that the treatments for such things are, expensive, moderately effective at best, and are overall inadequate.
New Study Explains why MS Affects more Women
MS affects women almost four times more often than it affects men. The reasons are unclear, but a new study is the first to associate a sex difference in the brain with MS. The newly identified difference between the brains of women and men with multiple sclerosis (MS) offer not only insight into why, but also may offer a course of treatment.
Looking at mice and people that have MS, the researchers found that females susceptible to MS produce higher levels of a blood vessel receptor protein [S1PR2]. than males and that the protein is present at even higher levels in the brain areas that MS typically damages.